Herniated Disc Treatment Without Surgery: A Conservative Approach
You Rarely Need Surgery for a Herniated Disc
If you’ve been diagnosed with a herniated disc and told you might need surgery, you’re likely frightened and uncertain about your future. Will you ever be pain-free again? Will you be able to return to your activities? Must you undergo an operation with all its risks, costs, and recovery time?
The good news is that the vast majority of herniated discs—even large ones causing significant pain and radicular symptoms—can be successfully treated without surgery. At the Physicians’ Back Institute, we’ve spent 30+ years helping patients with disc herniations avoid the operating room while achieving excellent functional outcomes through our comprehensive conservative approach.
Understanding Herniated Discs: What’s Really Happening
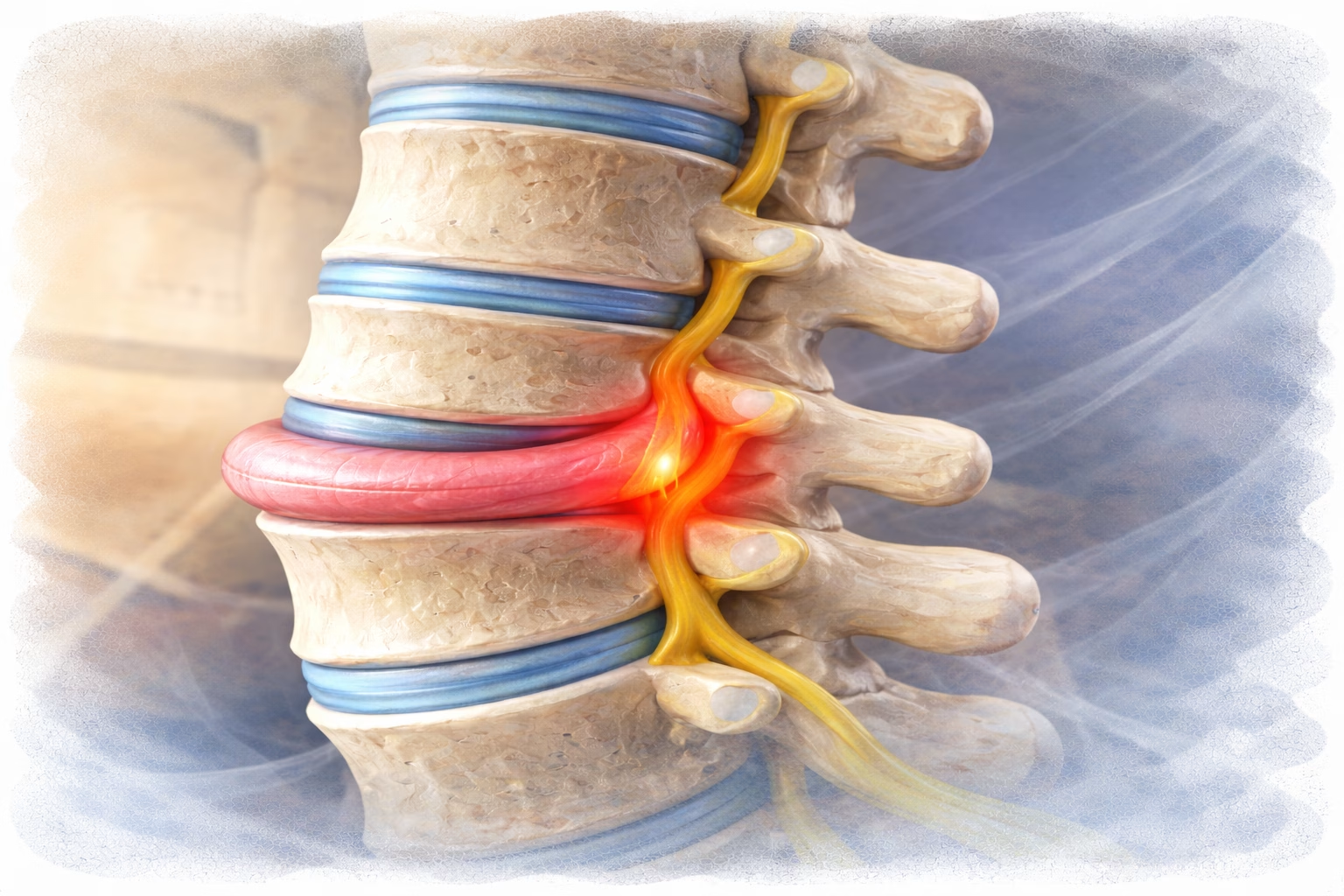
A herniated disc occurs when the gel-like center of a spinal disc (nucleus pulposus) pushes through a tear in the tougher outer layer (annulus fibrosus). This herniated material can compress or irritate nearby nerve roots, causing:
- Local back or neck pain
- Radiating pain down the arm (cervical herniation) or leg (lumbar herniation)
- Numbness, tingling, or weakness in the affected limb
- Reduced reflexes
- Difficulty with certain movements
What many patients don’t realize is that disc herniations are extremely common—studies show that 30-40% of people without any back pain have disc herniations visible on MRI. This means that your MRI findings don’t necessarily predict your symptoms or determine whether you need surgery. What matters is the functional impact and your body’s ability to heal.
Natural History: Most Herniated Discs Improve Without Surgery
Medical research consistently demonstrates that herniated discs tend to improve naturally over time, even without surgery:
- Studies show that 70-90% of patients with herniated discs and radicular symptoms improve significantly with conservative treatment.
- Disc herniations often resorb (shrink) naturally over 6-12 months as the body’s immune system breaks down the herniated material.
- Pain typically improves faster than disc size changes—meaning you can feel dramatically better while the disc is still visible on imaging.
- Long-term outcomes (at 1-2 years) are often similar between patients treated surgically and those treated conservatively.
This doesn’t mean surgery is never needed—but it does mean that giving conservative treatment adequate time to work is medically appropriate and often highly successful.
When Surgery Is Truly Necessary
Before discussing our conservative approach, let’s be clear about when surgery is genuinely indicated:
Emergent Situations: – Cauda equina syndrome (loss of bowel/bladder control, saddle anesthesia) – Progressive neurological deficit with severe weakness – Profound motor weakness that isn’t improving.
Relative Indications: – Severe pain that hasn’t improved after 6-12 weeks of comprehensive conservative treatment – Functional disability that makes basic daily activities impossible despite treatment – Patient preference for surgery after understanding all of the options and risks.
For the majority of patients, however, none of these situations apply, and conservative treatment is both appropriate and effective.
Our Comprehensive Conservative Approach
At the Physicians’ Back Institute, treating herniated discs isn’t about a single intervention—it is about a systematic, multi-faceted approach that addresses all the factors contributing to your pain and dysfunction.
1. Thorough Evaluation and Accurate Diagnosis
We begin with a comprehensive clinical examination to: – Confirm that your symptoms actually match your imaging findings – Identify which specific nerve root is affected – Assess the severity of nerve compression – Evaluate muscle strength, reflexes, and sensation – Identify contributing factors (muscle imbalances, joint restrictions, postural problems) – Determine if non-disc problems (SI joint, facet joints, muscle) are contributing.
Many patients diagnosed with “herniated disc” at other facilities actually have significant contributions from other structures that must be addressed for successful treatment.
2. Osteopathic Manipulation Therapy (OMT)
OMT is central to our treatment approach for disc herniations:
- Reducing nerve root irritation: Gentle techniques can reduce pressure on compressed nerves by improving spine function and reducing muscle spasm.
- Improving disc mechanics: Restoring proper motion to adjacent spinal segments reduces stress on the injured disc.
- Releasing muscle tension: Severe muscle guarding around a herniated disc creates additional pain and restriction; releasing this tension often provides immediate relief.
- Addressing compensatory dysfunction: Your body compensates for disc pain by altering movement patterns, creating secondary problems we must treat.
- Enhancing healing: Improved circulation and reduced inflammation support the natural healing process.
3. Targeted Exercise and Rehabilitation
Exercise is crucial, but it must be specific and properly timed:
- Directional preference: McKenzie-based approaches to determine which movements reduce your symptoms.
- Neural mobilization: Gentle exercises to reduce nerve irritation and adhesions.
- Core stabilization: Strengthening deep spinal stabilizers to protect the injured disc.
- Flexibility training: Addressing muscle tightness that contributes to disc stress.
- Functional retraining: Teaching proper movement patterns for daily activities.
We prescribe exercises based on your specific presentation, not generic protocols.
4. Ergonomic and Postural Correction
Many disc herniations occur because of repetitive stress from poor ergonomics:
- We analyze your work setup, sleeping positions, and daily habits.
- We identify positions and movements that aggravate your disc.
- We teach modified body mechanics that reduce disc stress during recovery.
- We provide strategies for long-term spine protection to prevent recurrence.
5. Activity Modification and Education
Understanding your condition empowers you to participate in your healing:
- We explain what’s happening in your spine and why you have pain.
- We teach you which activities to avoid temporarily and which you can continue.
- We help you understand the natural healing timeline.
- We address fears and misconceptions that might prevent optimal recovery.
- We set realistic expectations about the recovery process.
6. Adjunctive Treatments When Appropriate
Depending on your specific case, we may incorporate:
- Anti-inflammatory interventions: When appropriate, to reduce acute inflammation. In the acute phase, prednisone, a steroid, is frequently prescribed.
- Traction techniques: Gentle distraction to reduce disc pressure.
- Craniosacral therapy: For associated headaches or cervical issues.
- Visceral manipulation: When internal organ restrictions relating to their mobility and motility contribute to spinal tension.
- Coordination with physical therapy: For intensive exercise programs when indicated.
What to Expect During Recovery
Recovery from a herniated disc varies by individual but typically follows this pattern:
Weeks 1-2 (Acute Phase): – Focus on pain reduction and preventing worsening – Oral steroids. Gentle OMT to reduce muscle spasm and nerve irritation – Careful activity modification.
Weeks 3-6 (Subacute Phase): – Gradually increasing activity – More aggressive exercise prescription focused on strengthening of transversus abdominis, gluteus medius and maximus – Decreasing treatment frequency as you improve – Focus shifts toward restoration of function.
Weeks 6-12 (Rehabilitation Phase): – Progressive strengthening and return to normal activities – Continued exercise progression – Monthly follow-ups to monitor progress – Education on long-term spine health.
Months 3-12 (Resolution Phase): – Most symptoms resolved or minimal – Full return to activities – Maintenance exercise program – Periodic check-ins as needed.
Most patients see significant improvement within 6-12 weeks, with continued gains over 3-6 months.
Success Stories: Real Patients, Real Results
Over 30+ years, we’ve helped countless patients avoid surgery for herniated discs:
- Patients with significant lumbar disc herniations and severe sciatica who were surgical candidates, now pain-free and fully functional.
- Individuals with cervical herniations causing arm pain and weakness, who regained full strength without surgery.
- People who failed standard physical therapy elsewhere, but responded dramatically to our comprehensive approach.
These aren’t miraculous cures—they’re the natural result of giving your body the support it needs to heal through expert conservative care.
When Conservative Treatment Doesn’t Work
We’re honest about outcomes. If you don’t improve significantly after 2-3 weeks of comprehensive conservative treatment, we’ll have a candid discussion about whether surgery has become appropriate. Some patients do ultimately need surgery, and we maintain excellent relationships with skilled spine surgeons for referrals when necessary.
However, we’ve learned that many patients improve with our care precisely because we have the specialized skills and patience that conventional treatments lack. Saying “physical therapy didn’t work” isn’t the same as saying “comprehensive conservative treatment won’t work”—our approach is fundamentally different.
Take the Conservative Path First
If you have a herniated disc and are facing the possibility of surgery, we encourage you to explore expert conservative treatment first. Surgery is irreversible; conservative treatment carries no such risk. Even if you ultimately need surgery, trying conservative care first is medically appropriate and often avoids an operation. In case surgery is necessary, you will be better prepared to recover from it.
Don’t rush into surgery. Call (415) 776-4644 to schedule your comprehensive evaluation and discover if your herniated disc can be successfully treated without an operation.
