Spinal Stenosis
What is Spinal Stenosis?
One can have an active, pain free life. When seeking relief for spinal stenosis, surgery for control of symptoms is rarely necessary. It is never a long-term solution as the underlying condition remains. A rehabilitation program is important for everyone. – Drs. Irène & Robert Minkowsky
Stenosis means narrowing, and spinal stenosis indicates that there is narrowing of the spinal canal (central stenosis) or narrowing of the openings where spinal nerves exit the canal (foraminal stenosis). Although some individuals may be born with a congenitally narrow spinal canal, for the vast majority of individuals, spinal stenosis is a degenerative condition that occurs progressively over time. If we live long enough, we all develop it.
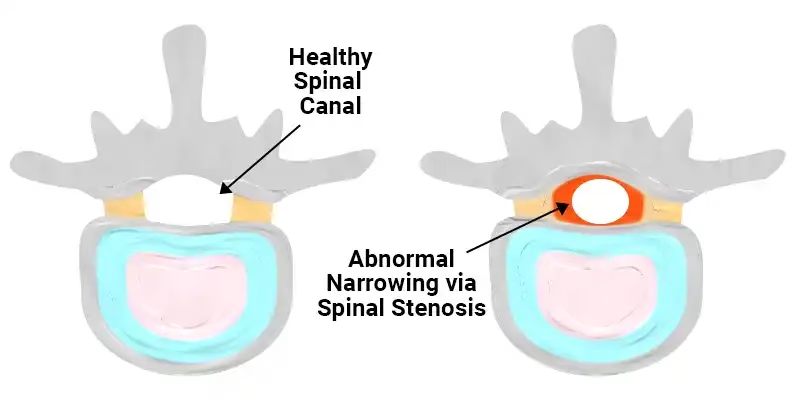
With intervertebral disc bulging, herniation or drying, the disc space is reduced, secondary arthritic change occurs in the facet joints and ligaments hypertrophy. The spinal canal or neural foramen is narrowed by these changes.
By the time we are 50, virtually everyone has some spinal stenosis, though for the majority it is asymptomatic. Symptoms from stenosis occur principally when nerve tissue is impacted, creating radicular symptoms of radiating pain down an arm or leg or back pain that occurs with standing or walking. Individuals with lumbar stenosis prefer to sit. Going to a museum or a cocktail party can provoke pain and the quality of life is affected. However, one can live pain free with spinal stenosis if there is balance in and around the spine and one performs specific exercises to open the canal and optimize function.
Spinal Stenosis Pain
If most individuals with stenosis are pain free, why and how do we get into trouble?
The main variables in stenosis are changes occurring in the disc and arthritis in the facet joints. Arthritic change occurs slowly. The disc, however, can bulge more from one moment to the next and it is this change that usually renders stenosis symptomatic. Triggers can include forward bending, lifting, arching of the back, traveling or other activities that load the disc or narrow the canal. In the neck, carrying or working with the arms overhead may stress the discs. Usually there are several factors that together get us into trouble.
If spinal stenosis becomes symptomatic, what are the treatment options?
There are 2 goals.
- Relieve the acute symptoms.
- Have a daily exercise program that optimizes the canal and the function of the spine, maintaining an individual in a symptom free state.
Acute Symptom Relief
With nerve or spinal cord compression, swelling occurs. This creates more compression and a vicious cycle begins. The first goal is to decrease swelling and relieve pressure on nerve tissue.
The treatment options include NSAIDS or oral prednisone. If these measures fail to improve symptoms, an epidural injection and selective nerve root block are often helpful. In this procedure, steroid is injected in the area of nerve tissue irritation. Although many patients view a steroid injection as a treatment cure to be repeated, in our experience, it is usually most helpful to decrease acute symptoms and enable an individual to get into a preventative rehabilitation program.
Along with the use of anti-inflammatory medication, instruction in isometric core muscle strengthening exercises, flexion exercises and passive traction in a 90-90-degree position to optimize canal size are essential.
Long Term Program
Most individuals with spinal stenosis can be maintained in a symptom free state over years if they are diligent in doing the exercise program that emphasizes strengthening of transversus abdominis (core) and flexion exercises. Avoiding extension, weight reduction, attention to posture and body mechanics and dynamic use of the abdominal muscles in activities of daily living are important as well.

Occasionally an individual may require surgery if they have progressive neurologic symptoms. However, the good news is that for the vast majority of individuals with spinal stenosis the treatment solution is a conservative one. One can have an active, pain free life. Surgery for control of symptoms is rarely necessary. It is never a long-term solution as the underlying condition remains. A rehabilitation program is important for everyone.
